Challenges of diagnosis and management of eczema in patients with skin of colour
Key Learnings
|
Which of the following patients would you diagnose with eczema?
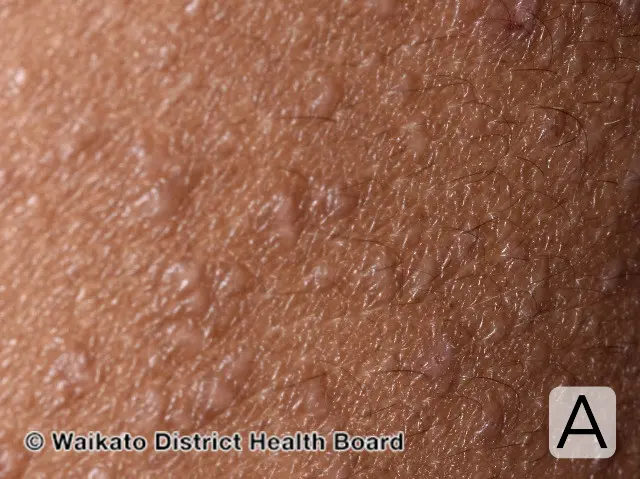




About the images
Image A Close-up of follicular atopic dermatitis
Image B Adhesive plaster reaction
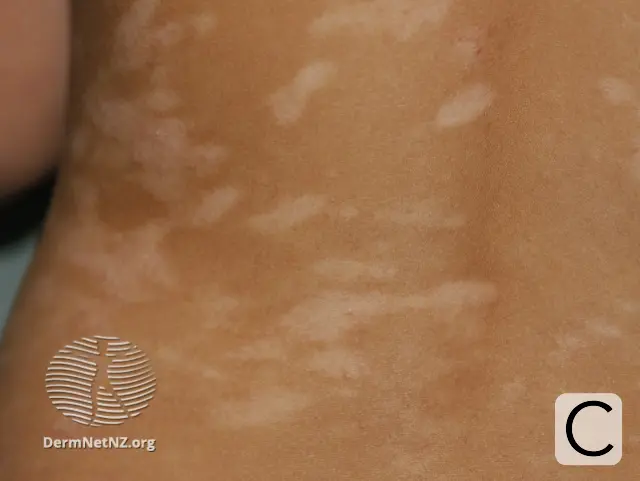
Image C Atopic dermatitis postinflammatory hypopigmentation
Image D Lichen Planus
Image E Bilateral cheek eczema; Dennie-Morgan folds are evident on the lower lids
Image F Scaly lichenoid patches of atopic dermatitis on the neck in patient with skin of colour
Primary care challenges of eczema in skin of colour
Eczema (atopic dermatitis, atopic eczema) is a common chronic, relapsing inflammatory skin condition that affects children and adults around the world, including about 2.8 million Australians.1
Most primary care health professionals are familiar with the classic presentation of eczema – recurrent, pruritic, poorly-demarcated erythematous patches with excoriation, predominantly affecting flexor surfaces.2 However, while this description defines eczema for people with lighter skin tones it is not adequate for diagnosis in people with skin of colour.
Skin of colour refers to skin that is ‘non-white’, typically occurring in people from ethnic and racial groups such as Asian, African, Latino, Mediterranean, Middle Eastern, and First Nations Peoples.3,4
Apart from differences in presentation, eczema in people with skin of colour has also been reported to occur with increased frequency, severity, and persistence compared to people with lighter skin tones.4,5 Yet these populations remain under-reported and under-represented in dermatology trials. Such absences in knowledge can impact the capacity of health professionals to provide appropriate care for people with skin of colour who have eczema, leading to misdiagnosis, underestimation of severity and delay in treatment.5,6
Dr Michelle Rodrigues MBBS (Hons), FACD, Consultant Dermatologist, The Royal Children’s Hospital, Melbourne, Vic; Honorary Senior Lecturer, The University of Melbourne, Melbourne, Vic; Founder, Chroma Dermatology.
How to improve care of eczema in skin of colour
Do not rely on erythema to assess severity
In patients with skin of colour, erythema is not a useful determinant of eczema inflammation.4,5 Lesions can often appear violaceous or grey rather than textbook red. In highly pigmented skin, erythema may be difficult to see, potentially masking the severity of the disease.5 Skin warmth, oedema and overlying scale may help health professionals to detect erythema in these cases.5,6
Current scoring tools such as SCORing Atopic Dermatitis (SCORAD), Eczema Area and Severity Index (EASI) or validated Investigator Global Assessment scale for Atopic Dermatitis (vIGA-AD), reflect ‘classic’ erythema as it presents in lighter skin tones. The Australasian College of Dermatologists (ACD) notes that care should be taken when using these tools for people with skin of colour, including Aboriginal and Torres Strait Islander people, as they may delay diagnosis or underestimate eczema severity in pigmented skin.7
The Eczema Management Algorithm developed in conjunction with and endorsed by the ACD recommends increasing the erythema score to avoid underestimation. This reflects similar recommendations made by the EASI authors and others, to increase the score by 1 grade or more in heavily pigmented skin.5,8,9
Think outside the textbook
Apart from erythema, there is a small but growing body of research showing that eczema is a heterogeneous condition that presents differently across ethnic and racial groups.4–6,10
For example, health professionals should be aware that:
-
there is a predominance for eczema to present as psoriasiform variants, with lichenified, well-demarcated, scaly lesions in individuals of East Asian heritage (e.g. Chinese, Japanese and Korean);5
-
there is a tendency for eczema to have extensor involvement, perifollicular accentuation and distinct papules in people of African heritage. Lichenoid variants have also been reported to be more common in this population and also those with Indian ethnicity (Figure 1).5
Secondary skin manifestations of eczema more likely to be seen in patients with skin of colour include:3–5
- Dennie-Morgan lines – a linear fold beneath the lower eyelid often with surrounding dyspigmentation (Figure 2);
- Labial melanocytic macules – pigmented macular freckling usually of the lower lip is reportedly a unique feature among people of Asian ethnicity;
- Palmar hyperlinearity – exaggerated linear markings on the palm;
- Prurigo nodularis – firm, pruritic, abraded, thickened, often dyspigmented nodules, have been described in people with Black skin (Figure 3).
Aboriginal and Torres Strait Islander peoplesResearch and insights about prevalence, disease burden and characteristics of eczema in Aboriginal or Torres Strait Islander people are limited. A recent systematic review looking at urban-living Indigenous children in multiple high-income countries found that current and severe symptoms of eczema were more common in Indigenous children compared with their non-Indigenous peers.11 However, there is little clinical research available to support diagnosis and management of eczema in this population. The 2nd edition of the National Healthy Skin Guidelines recently added a chapter on eczema, acknowledging that the condition is significantly intertwined with other skin infections such as impetigo, and may be missed when focus is on treating the acute presenting infection.12 The Perth Children’s Hospital has developed a practical toolkit to support the assessment and management of eczema in children with skin of colour and two Keeping our Mob Health eczema factsheets for children and parents. |
Consider differential diagnosis
Eczema is a clinical diagnosis made on presentation and patient history, without definitive diagnostic tests. There are a number of inflammatory skin conditions, infections, infestations and other diseases that may mimic, overlap or manifest as complications of eczema.3,13,14 Differential diagnoses that have been specifically noted as relevant to patients with skin of colour are:3,5,13,15
- seborrehic dermatitis
- psoriasis
- lichen planus
- lichen nitidus
- cutaneous T cell lymphoma
Proactively discuss potential pigmentation changes
In addition to the above-described presentations, people with darker skin tones who have eczema are also at higher risk for developing postinflammatory dyspigmentation (Figure 4).3,6 Dyspigmentation describes hyper- or hypopigmented skin around a present or previously inflamed eczematous lesion.3
Health professionals should appreciate that for some patients these changes to skin colour can be as distressing as having eczema. Make patients aware early in treatment that these changes may occur as the eczema resolves and reassure them that most cases resolve spontaneously with time (typically weeks to months) and without specific treatment.
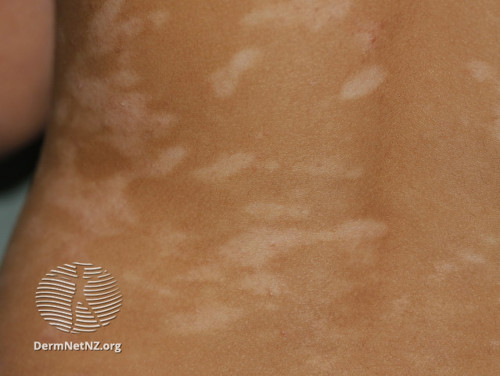 Figure 4. Atopic dermatitis postinflammatory hypopigmentation.
Figure 4. Atopic dermatitis postinflammatory hypopigmentation.Where a topical corticosteroid is involved for active flare management, emphasise the importance of treating to texture (smooth and itch-free) rather than appearance.
Chronic excoriation associated with severe eczema may result in permanent depigmentation in patients with darker skin.3,5
In cases where these changes are prolonged and becoming distressing to the patient or family, consider referral to a specialist dermatologist.
Dr Michelle Rodrigues
Consider ethnicity and culture to inform management
For all patients with eczema, the goals of care are to manage active flares, prevent future ones and improve skin barrier function.4–6 Essential actions to achieve these goals include:
- regular use of moisturiser;
- avoidance of personal eczema triggers;
- timely application of appropriate flare control treatments;
- acknowledging and addressing psychosocial concerns to improve quality of life and daily functioning;
- prevention and treatment of skin infections.
Current recommendations for the management of eczema are similar across ethnic groups, with minor nuances due to differences in skin phototype, genetics and cultural practices.3,5,6,16
For example, evidence suggests that Asian skin may be more reactive or sensitive than skin of other races. Moisturisers containing humectants such as urea, glycerine and propylene glycol may be more irritating and should be used with care in this group.3,5 Other studies have reported that Black skin has lower levels of ceramides, which may contribute to greater pruritis and dryness and hence require specific considerations when choosing suitable moisturisers.17
When discussing potential triggers, health professionals should remain aware that many cultures may have increased exposure to certain potential irritants due to practices and customs that involve food or plants as moisturisers (e.g. coconut oil), as medicines (e.g. Bush Medicine, Traditional Chinese Medicine, Ayurvedic medicine), or in the application of decorative dyes and tattoos (i.e. henna).4,6
Current Australian recommendations18,19 advise against:
-
moisturisers with food-derived proteins, (i.e. nuts, coconut, milk), especially if a person has broken skin and does not readily eat the food or has an allergy to it. This is particularly important in infants, because sensitisation to food and environmental allergens may occur through a broken skin barrier.
-
moisturisers with plant extracts or essential oils, i.e. lavender, rosemary and tea-tree.
While harm minimisation from these and other environmental triggers is important, discussions must be approached with sensitivity and respect for the person's culture, to build trust and optimise chances of treatment success.
In Australia, some cultural and ethnic subpopulations may also experience socioeconomic challenges to effective eczema care. Contributing factors include rurality and remoteness, limited access to appropriate healthcare resources and limited disposable income for treatment-associated costs.4 The National Healthy Skin Guideline notes that sorbolene cream is the most widely available moisturiser that is inexpensive and comes in large volume tubs.12 For eczema that requires topical corticosteroids, PBS streamlined authority numbers exist for prescription of increased quantities, which can facilitate adherence by reducing barriers to access.
Dr Michelle Rodrigues
Diagnosing and managing eczema in Australia’s ethnically and culturally diverse patients with skin of colour can be challenging. Health professionals need to look for clinical variations in presentation to reduce underdiagnosis or delayed care. Treatment should be proactive, to minimise inflammation and protect the skin barrier while also considering cultural practices. Clinicians should align skincare advice and prescriptions with each patient's cultural perspectives on skincare norms and treatment goals.
More on the quality use of medicines
QHUB is Medcast's new dedicated platform for education and resources that support safe and appropriate use of medicines.
Find out more
In-consultation resources
Educational activities and CPD
-
Podcast – Beyond Skin Deep: Unravelling the challenges of managing eczema
-
Webinar – The Eczema Equation: Burden of disease and challenges in management
References
Images A–F and Figures 1-4 have been sourced with permission from DermNet.https://dermnetnz.org/image-licence
1. Eczema Support Australia. (2023). The Burden of Eczema—Evidence for a National Strategy. Eczema Support Australia. www.eczemasupport.org.au/wp-content/uploads/2023/08/The-Burden-of-Eczema-Evidence-for-a-National-Strategy.pdf
2. Therapeutic Guidelines Limited. (2022, August). Atopic dermatitis. Dermatitis. https://tgldcdp.tg.org.au/viewTopic?etgAccess=true&guidelinePage=Dermatology&topicfile=c_DMG_Atopic-dermatitis_topic_1&guidelinename=auto§ionId=c_DMG_Atopic-dermatitis_topic_1#c_DMG_Atopic-dermatitis_topic_1
3. Gan, C., Brand, R., Foster, R. S., Weidinger, J., & Rodrigues, M. (2023). Diagnosis, assessment and management of atopic dermatitis in children with skin of colour. Australian Journal of General Practice, 52(10), 673–679. https://doi.org/10.31128/AJGP-01-23-6684
4. Courtney, A., Lopez, D. J., Lowe, A. J., Holmes, Z., & Su, J. C. (2023). Burden of Disease and Unmet Needs in the Diagnosis and Management of Atopic Dermatitis in Diverse Skin Types in Australia. Journal of Clinical Medicine, 12(11), 3812. https://doi.org/10.3390/jcm12113812
5. Gan, C., Mahil, S., Pink, A., & Rodrigues, M. (2023). Atopic dermatitis in skin of colour. Part 2: Considerations in clinical presentation and treatment options. Clinical and Experimental Dermatology, 48(10), 1091–1101. https://doi.org/10.1093/ced/llad162
6. Kaufman, B. P., Guttman-Yassky, E., & Alexis, A. F. (2018). Atopic dermatitis in diverse racial and ethnic groups—Variations in epidemiology, genetics, clinical presentation and treatment. Experimental Dermatology, 27(4), 340–357. https://doi.org/10.1111/exd.13514
7. The Australasian College of Dermatologists. (2021). Consensus statement: Management of atopic dermatitis in adults. Australiasian College of Dermatologists. https://www.dermcoll.edu.au/wp-content/uploads/2021/05/ACD-Consensus-Statement-Management-of-Atopic-dermatitis-in-adults-March-2021.pdf
8. Hanifin, J. M., Baghoomian, W., Grinich, E., Leshem, Y. A., Jacobson, M., & Simpson, E. L. (2022). The Eczema Area and Severity Index-A Practical Guide. Dermatitis: Contact, Atopic, Occupational, Drug, 33(3), 187–192. https://doi.org/10.1097/DER.0000000000000895
9. Perth Children’s Hospital. (2023). Key considerations for clinicians when assessing and managing children with atopic dermatitis who have skin of colour: A practical toolkit. https://pch.health.wa.gov.au/~/media/Files/Hospitals/PCH/General-documents/Health-professionals/PRGs/AD-SOC-clinician-toolkit.pdf
10. Gan, C., Mahil, S., Pink, A., & Rodrigues, M. (2023). Atopic dermatitis in skin of colour. Part 1: New discoveries in epidemiology and pathogenesis. Clinical and Experimental Dermatology, 48(6), 609–616. https://doi.org/10.1093/ced/llad111
11. Ricciardo, B. M., Kessaris, H., Kumarasinghe, P., Carapetis, J. R., & Bowen, A. C. (2023). The burden of atopic dermatitis and bacterial skin infections among urban‐living Indigenous children and young people in high‐income countries: A systematic review. Pediatric Dermatology, 40(1), 35–43. https://doi.org/10.1111/pde.15153
12. Telethon Kids Institute. (2023, October). National Healthy Skin Guideline For the Diagnosis, Treatment and Prevention of Skin Infections for Aboriginal & Torres Strait Islander Children annd Communities in Australia. https://infectiousdiseases.telethonkids.org.au/globalassets/media/documents/our-research/healthy-skin-arf/hsg-digital-18-10-2023.pdf
13. Siegfried, E. C., & Hebert, A. A. (2015). Diagnosis of Atopic Dermatitis: Mimics, Overlaps, and Complications. Journal of Clinical Medicine, 4(5), 884–917. https://doi.org/10.3390/jcm4050884
14. Napolitano, M., Fabbrocini, G., Martora, F., Genco, L., Noto, M., & Patruno, C. (2022). Children atopic dermatitis: Diagnosis, mimics, overlaps, and therapeutic implication. Dermatologic Therapy, 35(12), e15901. https://doi.org/10.1111/dth.15901
15. Adawi, W., Cornman, H., Kambala, A., Henry, S., & Kwatra, S. G. (2023). Diagnosing Atopic Dermatitis in Skin of Color. Dermatologic Clinics, 41(3), 417–429. https://doi.org/10.1016/j.det.2023.02.003
16. Alexis, A., Woolery-Lloyd, H., Andriessen, A., Callender, V., Gonzalez, M., Heath, C., & Han, G. (2022). Insights in Skin of Color Patients With Atopic Dermatitis and the Role of Skincare in Improving Outcomes. Journal of Drugs in Dermatology : JDD, 21(5), 462–470. Ovid MEDLINE(R) <2022>. https://doi.org/10.36849/JDD.6609
17. Alexis AF, Woolery-Lloyd H, Williams K et al. (n.d.). Racial/Ethnic Variations in Skin Barrier: Implications for Skin Care Recommendations in Skin of Color. Journal of Drugs in Dermatology, 20(9), 932–938. https://doi.org/doi:10.36849/JDD.6312
18. ACD-Consensus-Statement-Management-of-Atopic-dermatitis-in-adults-March-2021.pdf. (n.d.).
19. National Allergy Council. (2023). Managing eczema in children: A health professionals guide to moisturisers and corticosteroids. National Allergy Council. https://nationalallergycouncil.org.au/images/doc/Health_professionals_eczema_guide_about_moisturisers_and_steroids.pdf

The Quality Use of Medicines Alliance is a unique consortium of health sector organisations representing quality use of medicines expertise, education providers, researchers, colleges, peak bodies, member-based organisations, and consumer groups. Funded by the Australian Government under the Quality Use of Diagnostics, Therapeutics and Pathology (QUDTP) Program.
GP Dr Kate Annear and Clinical Psychologist A/Prof Aliza Werner-Seidler discuss practical strategies for engaging young people, conducting psychosocial assessments, and using lifestyle, social, psychological and digital interventions to support mild to moderate depression and anxiety in young people.
With one in three young Australians experiencing a mental health condition each year, and suicide remaining the leading cause of death for 16 to 24-year-olds, the way clinicians approach antidepressant use in teens and young adults has never been more important.
Discover practical strategies for GPs to identify and manage anxiety and depression in adolescents, balancing non-pharmacological care with thoughtful, evidence-based prescribing when needed. Find out how the Quality Use of Medicines Alliance is helping health professionals navigate this complex area with new clinical tools, national education programs and expert-led insights.



