Clinical Opal #2 - Painful Leg
Dave is a 33-year-old carpenter who presents to you with a painful red leg. It started about 48 hours previously as a red area and since then has spread and is now very painful. He feels unwell and says he has had a fever. Dave is generally well with no past medical history and is on no regular medications. He wonders whether something has bitten him.
One examination, Dave has a temperature of 38.6 and his leg appears as below. The area is hot and very tender to palpation.
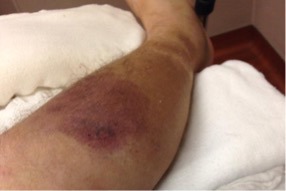
What uncommon but serious diagnosis must be considered in Dave?
Necrotising fasciitis is the diagnosis that must be considered and excluded in a presentation like Dave.
Necrotising fasciitis is a bacterial infection of the soft tissue and fascia and is a surgical emergency requiring urgent and aggressive management. While often spontaneous, it may follow penetrating or crush injury, or surgical procedures. In children, necrotising fasciitis S. pyogenes can follow varicella infection. Risk factors include age, diabetes, obesity, immune suppression and malignancy.
The cardinal clinical feature of necrotising fasciitis is pain disproportionate to the degree of redness. More advanced cases include bullae, obvious skin necrosis and crepitus. Patients need urgent admission for IV antibiotics and debridement.
References
- Therapeutic Guidelines https://tgldcdp.tg.org.au/etgAccess
- DermNET NZ https://dermnetnz.org/topics/necrotising-fasciitis/
- Necrotising fasciitis BMJ2020; 369 doi: https://doi.org/10.1136/bmj.m1428
Emergencies in General Practice
If you liked this Clinical Opal you will love our Emergencies in General Practice course. Sign up today for an essential evidence update on the recognition, investigation and management of common emergencies that present in General Practice. Click here for live webinar dates and other course information.

Simon is a GP based in Newcastle, NSW, and a senior medical educator with Medcast. He also has medical education roles with the RACGP and GPSA.
Over the past three decades, Simon has worked in clinical and educational roles in NSW and the NT, as well as in the Republic of Ireland. He has published over 75 peer reviewed journal articles, and in 2018 received the RACGP Corliss award for his contribution to medical education.
Simon is passionate about high quality education and training. He has particular interests in GP supervisor professional development and the rational use of tests and medicines. He is a proud member of Doctors for the Environment. He spends his spare time drinking craft beer and pretending that he is a musician in the Euthymics, an all-GP band.
Become a member and get unlimited access to 100s of hours of premium education.
Learn moreMarjory is a 68 year old in-patient who is 2 days post hip replacement. She is on rivaroxaban (xarelto) for VTE prophylaxis. You find her sitting on the floor of the bathroom, alert but in pain.
We explore the case of Edward, a patient with acute kidney injury (AKI), focusing on renal protection strategies. It explores fluid management, blood pressure control, nephrotoxic drug adjustments, and electrolyte monitoring. Treatment considerations include vasoactive medications, dialysis options like CRRT, and medication dosing to support renal recovery and prevent complications.
James, a university student with a history of seasonal allergic rhinitis, presents with sudden respiratory distress following exposure to grass pollen during a soccer game shortly before a summer thunderstorm. Could this be thunderstorm asthma?
